Blog
Teach Postpartum Hemorrhage With High-Fidelity Simulation
Postpartum Hemorrhage (PPH) is one of the leading causes of maternal mortality in the United States, yet many aren’t aware that an estimated 66-93% of PPH-related maternal deaths are preventable (Gyamfi-Bannerman et al., 2018).
These numbers are jarring and even more alarming when you learn that the United States ranks last in maternal-fetal healthcare among industrialized nations (Declercq & Zephyrin, 2020). A deeper dive into the statistics shows the stark disparity between minority groups–especially non-Hispanic Black women–whose maternal mortality rate is 2-3 times higher than non-Hispanic White women (Hoyert, 2021).
Uterine atony or the inability of the uterus to contract after birth is the primary cause of PPH, accounting for 70-80% of all hemorrhages (Wormer et al., 2021). While there are many risk factors for PPH, many cases involve “Inadequate monitoring, failure to escalate care in the setting of abnormal vital signs, communication miscues, suboptimal coordination with consultants, and the lack of timely involvement of senior clinicians” (Gyamfi-Bannerman et al., 2018). Hands-on clinical experience within the maternity unit is hard to come by and even more difficult for male students who are often excluded from observation. Many institutions are looking toward high-fidelity simulations to aid in educating their learners about PPH and how to treat the condition in emergent situations.
“The fear of the unknown on the Labor and Delivery unit can block their ability to learn. Having the ability to prepare them in advance, utilizing simulation, helps to build their confidence for when they get into the clinical setting and must take care of a real patient.”
Barbara Butynski MSN, RN, CPN
Boston Medical Center
Nursing Faculty/Clinical Instructor
High-fidelity simulations improve a learner’s competency and confidence, providing context and meaning to didactic learning (Richardson & Claman, 2014). Additionally, using simulated participants (actors) in simulation increases its fidelity even more; because the learner is having to interact with the patient while working through the problem at hand.
Due to the lack of clinical obstetric emergency experience within nursing programs, many learners are left with a learning gap entering the workforce. 20% of women who experience PPH have no risk factors (Evensen et al., 2017). Recognition of the symptoms associated with PPH, including uterine atony, is key to preventing intensive hemorrhaging and leads to experts engaging in timely intervention. Learners must be able to reenact emergencies such as PPH to develop the skills necessary to execute a contingency plan (Nathan, 2018). High-fidelity simulations allow educators to teach PPH step-by-step. The freedom to slow down or speed up simulations while learning these recognition signs also allows educators the ability to review contingency plans and intervention techniques at a pace necessary for learners to retain information. Such intervention techniques include fundal massaging, which reduces bleeding and cramping in the uterus as the uterine muscles contract.
“I think one of the strongest points of simulation—especially OB—you’ve got so many scenarios where life-and-death literally hangs in the balance. In clinical situations like postpartum hemorrhage or shoulder dystocia, the stakes are too high to allow a student to provide care and critically think through the situation when it’s a live human being. By combining Avbirth and a standardized patient in the simulation, it’s going to be that much more realistic.”
Marilynn Murphy DNP, RN, CHSE, CNE
Simulation Lab Coordinator
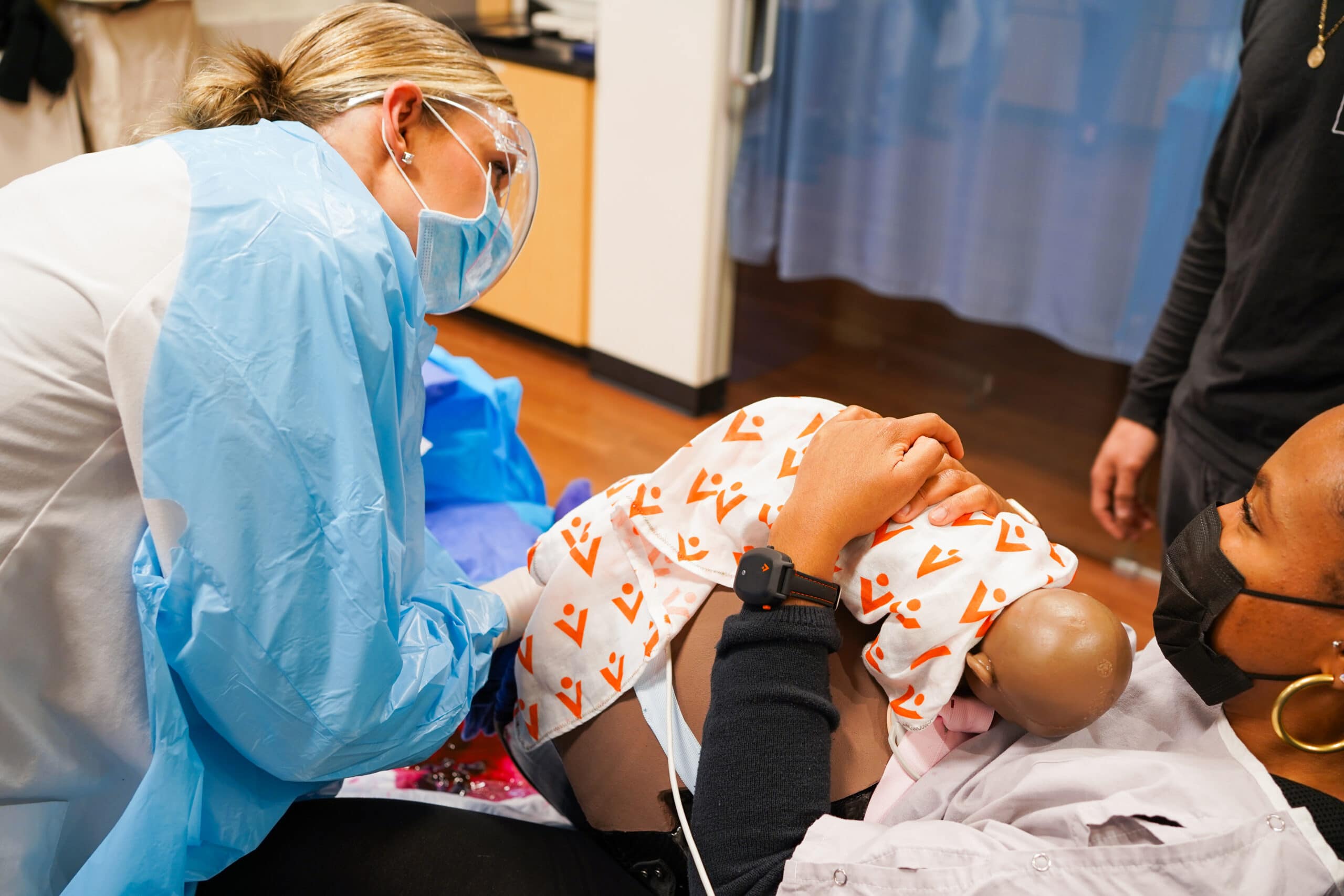
Avkin’s Research & Development team—partnering with Lifecast/Echo Healthcare for their full-term infant and iSimulate for their CTGI fetal heart monitor—created Avbirth, a wearable birthing simulation that provides learners with the opportunity to reenact normal and abnormal birthing scenarios as well as obstetric emergencies. With Avbirth, the learner will not only be able to apply what they learned in the classroom; but they will also be able to communicate with a patient, practice their skills, and learn from their mistakes within a controlled environment.
To learn more about Avbirth or to see a live demonstration click here.
