Blog
Closing the Practice Gap, Wound Care
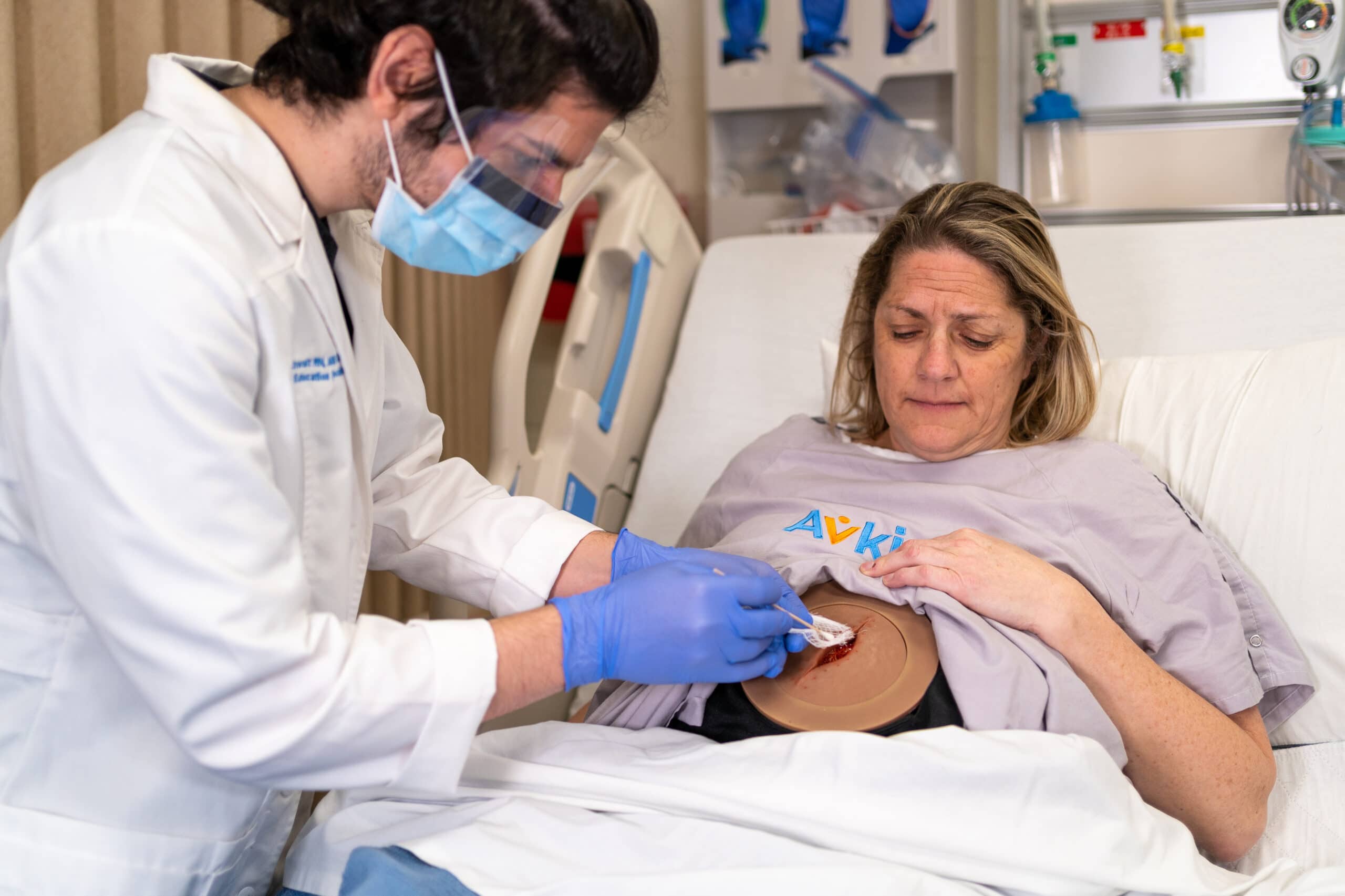
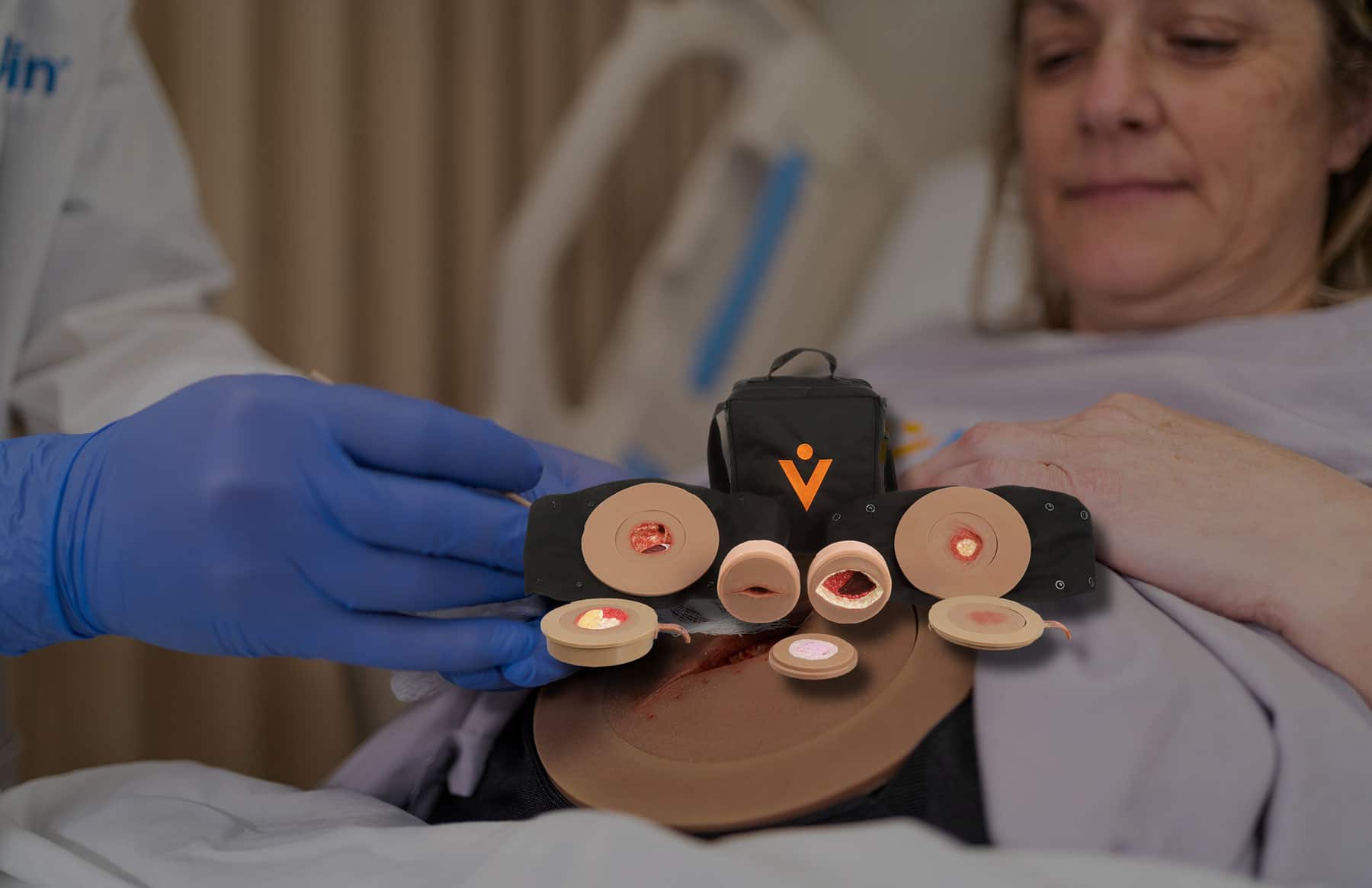
With pressure injuries (PI) as a major concern for patient safety and the cost of patient care, Ayello et al. suggest nursing programs should seek out faculty with specific knowledge in wound care (Ayello, Zulkowski, Capezuti, Jicman, & Sibbald, 2017). Learners should not leave education programs without the skills and knowledge to identify, care for, and prevent pressure injuries. As new graduate nurses move into the clinical setting, ongoing education and training would further improve confidence and comfort with identifying, assessing, and caring for pressure injuries. These education initiatives would be well served to use Just in Time training, simulation modalities that include realistic wound assessment, staging, and care, and knowledgeable preceptor bedside experiences during clinicals, onboarding, and orientation to address this preparation to practice gap (Ayello, Zulkowski, Capezuti, Jicman, & Sibbald, 2017).
Another factor affecting the preparation to practice gap is that skin tone diversity is poorly discussed in education programs (Oozageer Gunowa, 2020). Failure to discuss the diversity of skin tones continues the racial disparities rampant in healthcare today. Educators must actively seek out better methods to prevent color blindness in their learners. This may be accomplished by acknowledging and creating an open conversation about the spectrum of skin tones seen in all patients while updating education to include specific discussion on skin tones. Oozageer Gunowa, et al, explains that there is a skin tone spectrum that must be considered in the assessment of patient skin, in the prevention and treatment of pressure injury. Reflective practice is one avenue to consider when attempting to change structural racism in education. Currently, this is woefully inadequate for preparing learners to practice and feeding an ever-present disparity for darker skin-toned individuals (Oozageer Gunowa, 2020).
Medical Device Related Pressure Injury (MDRPI) has been deemed preventable by proper assessment and constant checking. Are we encouraging and teaching critical thinking for our new nurses – how might PI be prevented in this patient with these specific needs? When the preparation to practice gap is not minimized, there are going to be errors. There will be pressure ulcers/injuries. Guilt and hopelessness ensue (Tan, Cheng, Hassan, He, & Wang 2020). While most agree the responsibility for skin health likes with all healthcare team members. The nurse holds the proverbial bag, especially when the outcome is poor.
“…strong and thoughtful leadership among nursing leaders and senior nurses is necessary to supervise, educate and test the knowledge of ward nurses on MDRPI prevention. Nursing leaders can cultivate a sustainable healthy culture among all nurses to share associated challenges, take ownership and reflect on areas for improvement. (Tan, Cheng, Hassan, He, & Wang 2020)
The cost of continued theory to practice gap, with a focus on PI, is astronomical. The cost of Hospital Acquired Pressure Injuries (HAPI) is estimated to be BILLIONS of dollars per year in the United States alone (Padula, 2019). Add this cost to the cost of attrition and burn out and the total becomes even more insurmountable. Providing relevant training before graduation, with a focused onboarding and precepting in the clinical environment is necessary to begin to bridge this gap and appropriately care for patients.
Providing new and innovative ways to bridge the preparation to practice gap can be improved by adding communication and assessment skills to training. The use of wearable simulators and allows learners to incorporate communication, critical thinking, and assessment into training and learn to treat, as they already do or eventually will, a human patient.
Learn more about Avwound
References
Ayello, E. A.-B., Zulkowski, K. D., Capezuti, E. P., Jicman, W. H., & Sibbald, R. G. (2017, February). Educating Nurses in the United States about Pressure Injuries, Advances in Skin & Wound Care. Advances in Skin & Wound Care, 30(2), 83-84. doi: 10.1097/01.ASW.0000511507.43366.a1
Oozageer Gunowa, N. B. (2020, October 12). Embedding skin tone diversity into undergraduate nurse eduation: Through the lens of pressure Injury. Journal of Clinical Nursing, 29, 4358-4367. doi:DOI: 10.1111/jocn.15474
Padula, W. D. (2019). The national cost of hospital-acquired pressure injuries in the United States. 16, 634-640. doi:10.1111/iwj.13071
Tan JJM, Cheng MTM, Hassan NB, He H, Wang W. (2020, July). Nurses perception and experiences towards medical device-related pressure injuries: A qualitative study. Journal of Clinical Nursing, 29(13-14), 2455-2465. doi:DOI: 10.1111/jocn.15262